Obesity is a medical condition in which a person has an excessive amount of body fat that increases their risk of health problems.
While it is often associated with body weight, it is more accurately understood as a metabolic and hormonal disorder that influences energy use, appetite, and fat storage.
What Causes Obesity?
Obesity is usually assumed to be a result of too much fat in the body due to eating too much and moving too little. However, it is actually more complex than that.
Body weight is regulated by a network of hormones and metabolic processes. When these systems are disrupted, the body may store more fat, slow down energy use, or increase hunger signals.
One of the key drivers is insulin resistance, where the body becomes less responsive to insulin and starts storing more fat, particularly around the abdomen.
Certain medical conditions can also contribute to the problem. For example, hypothyroidism can slow metabolism, while polycystic ovary syndrome may affect weight through hormonal imbalance and changes in insulin sensitivity.
Lifestyle factors still play an important role. A combination of biological, behavioural, and environmental influences—such as diets high in processed foods and sugar, lack of physical activity, poor sleep, and chronic stress can all contribute to weight gain. Genetics and age-related changes in metabolism may also make some individuals more prone to gaining weight than others.
In most people, obesity develops from a combination of these factors rather than a single cause.
Symptoms and Diagnosis of Obesity
There are no specific symptoms of overweight and obesity. Your healthcare provider may diagnose overweight or obesity based on your medical history and an elevated Body Mass Index, also known as BMI.
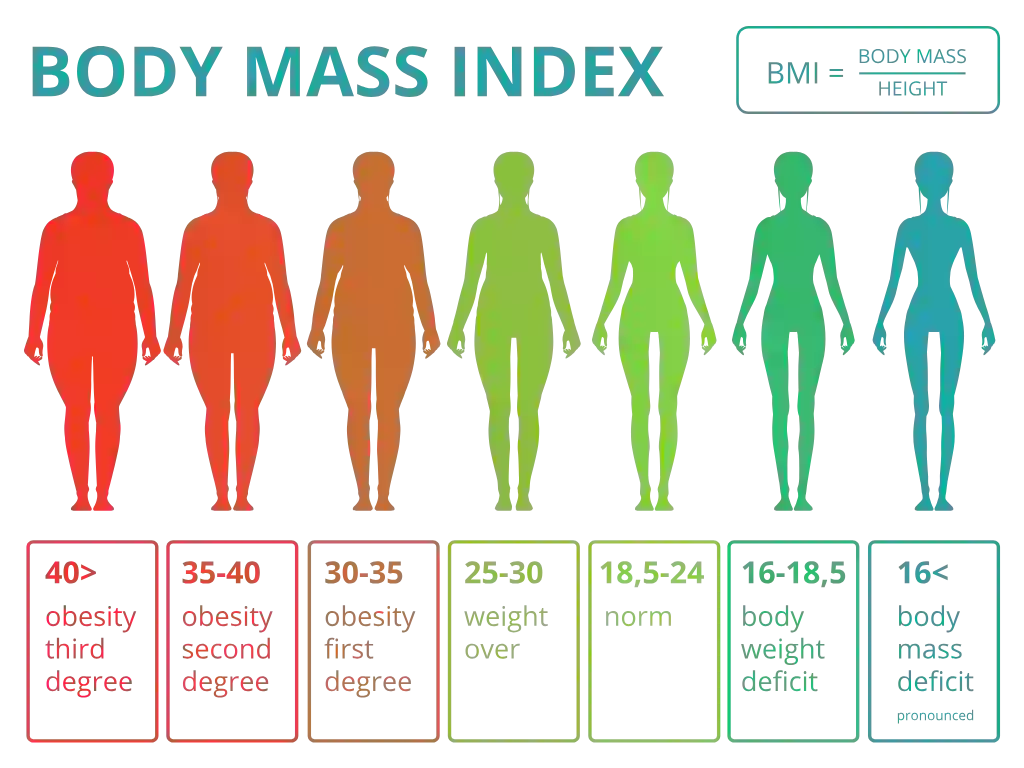
It is calculated by dividing your weight in kilograms by your height in meters squared.
However, BMI is only a screening tool. It does not distinguish between fat and muscle, nor does it reflect how fat is distributed in the body. In clinical practice, doctors may also assess waist circumference and recommend blood tests to evaluate metabolic health. These tests can help detect early changes in blood sugar, cholesterol levels, and thyroid function.
Risk Factors
Obesity is usually the result of several overlapping factors rather than a single cause. The key risk factors may include:
- Eating high-calorie or processed foods
- Drinking beverages that are high in sugar
- Poor sleep
- Chronic stress
- Family history of obesity
- Hormonal conditions such as hypothyroidism or PCOS
- Certain medications
Complications (Health problems caused by obesity)
Obesity is a chronic condition that can affect nearly every organ system in the body. People who are overweight or obese are at greater risk of developing chronic diseases such as:
Type 2 diabetes mellitus
Type 2 diabetes mellitus occurs when blood glucose levels become too high. Many individuals with type 2 diabetes mellitus are overweight or obese. Over time, raised blood sugar can lead to serious complications such as heart disease, stroke, kidney damage, vision problems, and nerve damage.
Losing just 5 to 7 percent of your body weight can significantly reduce your chance of developing type 2 diabetes mellitus.
Hypertension
High blood pressure, or hypertension, occurs when blood flows through the vessels with excessive force.
If left untreated, it raises the risk of heart attack, stroke, and kidney disease. Reaching a healthy weight can help lower blood pressure and reduce these risks.
Sleep apnoea
Sleep apnoea is a common condition in which the upper airway becomes blocked during sleep, causing irregular breathing or brief pauses in breathing.
If left untreated, sleep apnoea increases the risk of heart disease, diabetes mellitus, and other serious health problems.
Fertility problems
Hormonal balance can also be affected. In men, it is linked to lower sperm count and reduced sperm quality. In women, it can disrupt the menstrual cycle and ovulation, making it harder to conceive or carry a pregnancy to term. Obesity may also reduce the success of certain fertility treatments.
Treatment and Management Options
Managing obesity is not about quick fixes or extreme dieting. Instead, the focus is on improving overall health in a sustainable way.
Lifestyle modification
A structured lifestyle plan focuses on sustainable, realistic changes rather than extreme dieting.
Balanced nutrition: Reducing daily intake by about 500 to 750 calories can support gradual weight loss of 0.5 to 1 kg per week. As a general guide:
- Women: around 1,200 to 1,500 calories per day
- Men: around 1,500 to 1,800 calories per day
Focus on vegetables, fruits, whole grains, and lean proteins such as fish, poultry, tofu, and beans. Limit sugary drinks, fried foods, and large portions.
Exercise: Aim for at least 150 minutes of moderate activity weekly, such as brisk walking, cycling, or swimming. Include strength training two to three times per week to maintain muscle mass.
Even a 5 to 10 percent weight loss can significantly improve overall health.
Behavioral support
Counselling or structured programs can help address emotional eating, stress, and long-standing habits.
Medical therapy
In selected cases, prescription medications may be used to support weight loss under medical supervision.
Surgical options
For individuals with severe obesity or obesity-related complications, bariatric surgery may be considered after careful evaluation.
Importantly, treatment plans should be personalised, taking into account medical history, lifestyle, and long-term goals.
When Should You See a Doctor
You should consider seeking medical advice if you:
- Have a BMI in the overweight or obese range
- Experience breathlessness or joint pain
- Have a family history of diabetes mellitus or heart disease
- Notice rapid or unexplained weight gain
- Struggle with weight despite conscious lifestyle efforts
Early assessment can help identify underlying causes and prevent more serious complications from developing over time.
Book an AppointmentFrequently Asked Questions About Obesity
Yes, poor sleep can increase the risk of obesity. It disrupts hormones that control hunger, making you feel hungrier and more likely to overeat.
Obesity is a recognised medical condition. While lifestyle factors such as diet and activity levels play a role, it is also influenced by how the body regulates hormones, metabolism, and energy use. In many cases, underlying metabolic or hormonal imbalances contribute to weight gain and difficulty losing weight.
Hormones help regulate appetite, metabolism, and fat storage. When these are out of balance, the body may increase hunger, reduce energy expenditure, or store more fat.
Weight loss can be challenging when the body is affected by hormonal factors. For example, insulin resistance can make the body store more fat, while conditions like hypothyroidism may slow metabolism. These factors can make standard diet and exercise approaches less effective without medical support.
Doctors may recommend a combination of physical measurements and blood tests. These can include BMI, waist circumference, blood glucose levels, cholesterol profile, and thyroid function tests. These assessments help identify underlying metabolic or hormonal issues.
Weight loss medications can be safe and effective when prescribed appropriately and monitored by a doctor. They are usually recommended for individuals with obesity-related health risks or when lifestyle changes alone are not sufficient.
Genetics can influence how the body stores fat and regulates appetite, but it is usually not the only factor. Environmental and lifestyle factors, along with hormonal regulation, also play a significant role.
You may consider seeing an endocrinologist, especially if your weight may be influenced by underlying hormonal or metabolic factors.
Endocrinologists specialise in conditions that affect metabolism and hormone balance. They can provide a comprehensive evaluation and recommend personalised treatment options.
In some cases, a general practitioner may also be a good first point of contact, particularly for initial assessment and guidance.








