Insulin resistance is a metabolic condition in which the body’s cells do not respond effectively to insulin.
Under normal conditions, insulin helps move glucose (sugar) from the bloodstream into the cells, where it is used for energy. When this process becomes less efficient, the body compensates by producing more insulin. Over time, this can lead to consistently high insulin levels in the blood.
This imbalance can affect how the body stores fat, regulates appetite, and maintains energy levels. If left unmanaged, insulin resistance may increase the risk of developing type 2 diabetes mellitus and other metabolic conditions.
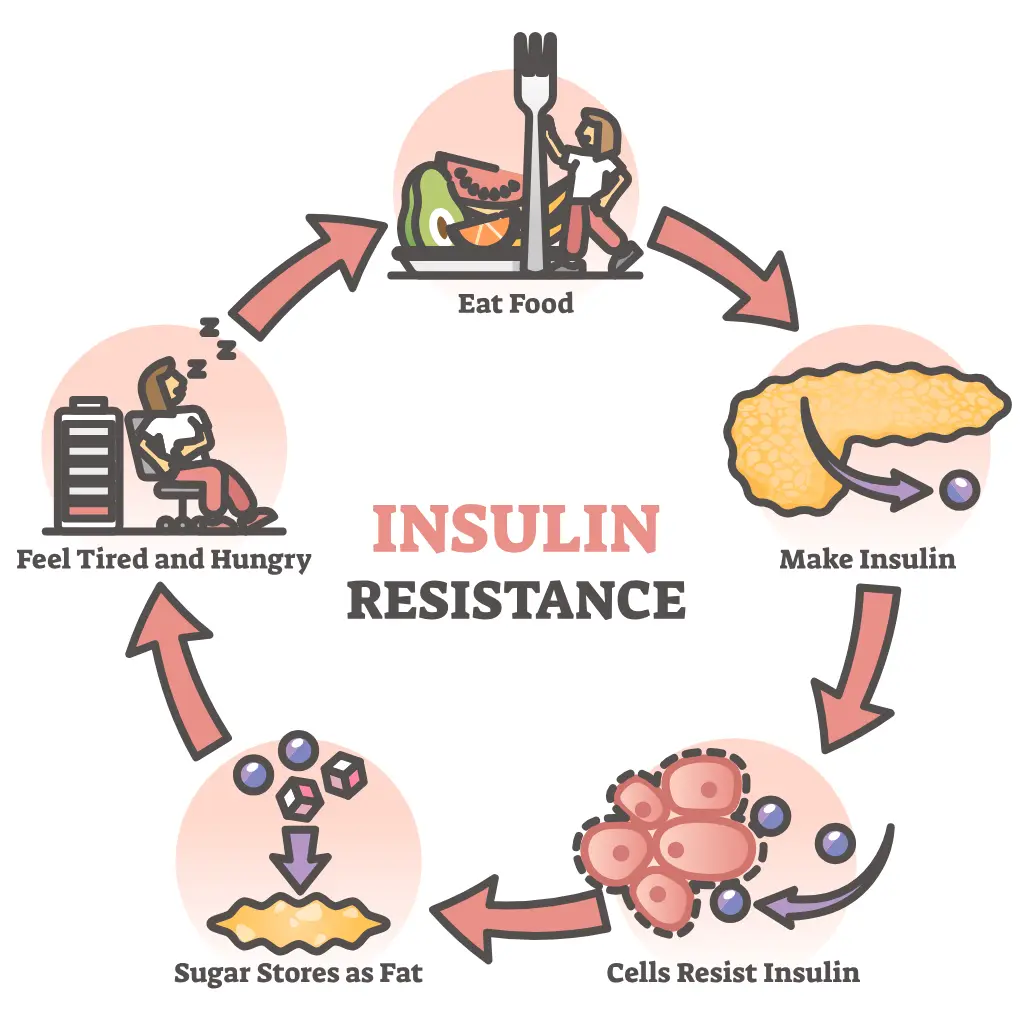
Insulin resistance is a common condition, particularly in individuals with excess body weight or those who are sedentary. It is also a key feature of metabolic syndrome.
One challenge is that many people may have insulin resistance without realising it. It often develops gradually and may not cause noticeable symptoms in the early stages.
Signs and Symptoms
In its early stages, insulin resistance may not cause obvious symptoms. However, some people may notice:
- Increased fat around the abdomen
- Difficulty losing weight despite lifestyle changes
- Persistent fatigue or low energy levels
- Increased appetite, particularly cravings for sugary foods
- Frequent urination
- Increased thirst
- Darkened patches of skin around the neck, underarms, or groin
These skin changes are known as acanthosis nigricans and can be a visible sign of underlying metabolic imbalance.
Causes & Risk Factors
Insulin resistance may develop due to a combination of metabolic, lifestyle, and genetic factors.
Common causes may include:
- Excess body fat particularly around the abdomen
- Physical inactivity
- High intake of carbohydrates and sugar
- Poor sleep quality
- Chronic stress
- Family history of diabetes mellitus
Certain medications and medical conditions may also contribute, including long-term steroid use and some treatments for chronic conditions.
Diagnosing Insulin Resistance
Diagnosing insulin resistance can be quite challenging, as there is no single test that confirms it directly. Instead, doctors assess a combination of clinical findings and laboratory results.
These may include:
- Fasting blood glucose levels: This test can screen for prediabetes and type 2 diabetes mellitus.
- HbA1c: Reflects average blood sugar levels over the past 2-3 months.
- Lipid profile (cholesterol levels): A group of tests that measures cholesterol and triglyceride levels
Together, these tests help evaluate how well the body is managing blood sugar and identify early signs of metabolic dysfunction.
Management & Treatment

How is Insulin Resistance Treated?
Not all factors that contribute to insulin resistance can be treated, such as genetic factors and age. However, insulin resistance can often be improved through lifestyle modifications:
Dietary changes
- Reducing intake of refined carbohydrates and sugary foods
- Emphasising whole foods such as vegetables, lean protein, and whole grains
Physical activity
- Regular exercise helps improve insulin sensitivity
- A combination of aerobic exercise and strength training is recommended
Weight management
- In some cases, weight loss may improve insulin resistance. Even modest weight loss can significantly improve insulin resistance.
These changes can help reduce insulin resistance, lower blood glucose levels, reduce bad cholesterol levels and raise good cholesterol levels instead.
Medical Treatment
In some cases, medication may be prescribed to improve insulin sensitivity or manage associated conditions.
Treatment is usually tailored based on individual risk factors and overall metabolic health.
Specialist Care
Because insulin resistance is closely linked to hormonal and metabolic function, patients may benefit from evaluation by an endocrinologist, particularly if symptoms persist or are associated with other conditions.
Possible Complications
If left untreated, insulin resistance can lead to several long-term health complications, including:
- Type 2 diabetes mellitus
- Metabolic syndrome
- Hypertension
- Increased risk of cardiovascular disease
Early intervention can significantly reduce the risk of these complications.
When to See a Doctor
You should consider seeing a doctor if you:
- Have difficulty losing weight despite lifestyle changes
- Experience persistent fatigue or increased hunger
- Notice darkened skin around the neck or underarms
- Have a family history of diabetes mellitus
- Have been told you have high blood sugar or abnormal cholesterol levels
Early assessment allows for timely management and helps prevent progression to more serious metabolic conditions.
Book an AppointmentFrequently Asked Questions About Insulin Resistance
No. Insulin resistance is a condition in which the body does not respond well to insulin, while diabetes mellitus occurs when blood sugar levels become persistently elevated. Insulin resistance often develops before diabetes mellitus.
In many cases, insulin resistance can be improved with lifestyle changes such as diet, exercise, and weight management. Early intervention is key.
You may consider consulting an endocrinologist, who specialises in metabolic and hormonal conditions. They can assess underlying causes and recommend a personalised treatment plan.
Yes. It is closely associated with conditions such as Polycystic Ovary Syndrome and Metabolic Syndrome and increases the risk of developing diabetes mellitus and cardiovascular disease.